In The News

07 January 2026
Investigator Kamena Kostova, named ‘Cell Scientist to Watch’
From the Journal of Cell Science, Investigator Kamena Kostova named a 'Cell Scientist to Watch'
Read Article
News
KANSAS CITY, MO—With its abundance of stem cells known as neoblasts, and remarkable abilities to restore body parts lost to injury, the humble flatworm, or planaria, has become an exciting model organism to study the processes of tissue and organ regeneration.
In two new studies, researchers in the laboratory of Howard Hughes Medical Institute Investigator Alejandro Sánchez Alvarado, Ph.D., at the Stowers Institute for Medical Research explore the intricate processes at work when stem cells differentiate into planarian skin cells.
Stowers researcher Elizabeth Duncan, Ph.D., and her collaborators provide one of the first in-depth in vivo investigations of chromatin regulation in planaria in a study published in the Dec. 17 online issue of Cell Reports. The research builds on Duncan’s investigations involving chromatin—a cluster of DNA, histones and non-histone proteins found within the nucleus of a cell. Chromatin packages DNA and acts as a gatekeeper of genetic information. During chromatin regulation, enzymes add chemical tags to the cell’s histone proteins, a process that predisposes regions of the genome to particular functions.
Duncan identified the key regions of the genome targeted by two such enzymes, Set1 and MLL1/2, by knocking down the levels of these enzymes in planarians. She found that the Set1 targets were largely associated with the maintenance of the planarian stem cell population and that worms without this enzyme eventually died. However, knocking down MLL1/2 produced strikingly different results; rather than losing stem cells, these planaria lost the cilia on their skin and stopped swimming.
Next, Duncan isolated planarian cells and analyzed histone protein interactions with DNA over the entire genome using chromatin immunoprecipitation followed by DNA sequencing (ChIP-seq). The paper is the first published report of the use of this technique in planaria. Using ChIP-seq, she marked the genes the enzymes targeted, revealing that changes in cilia-associated genes occurred in the neoblasts.
“That was the study’s biggest surprise,” Duncan says. “I wasn’t particularly thinking in the case of MLL1/2 that the genes would be affected in the adult stem cells. I might have guessed that they would be affected in the epithelial tissue where the cilia are.”
Cilia in planaria are similar to the cilia lining human lungs, which help expel mucous. Duncan’s discovery suggests that defects in ciliogenesis, the process of building cilia, may begin earlier than thought, a finding that has potential implications for a broad range of human health conditions, including primary ciliary dyskinesia, hydrocephalus, polycystic liver, and kidney disease and heart defects.
“Now we think that the stem cells may be preparing themselves to express cilia-coding genes later, and so this enzyme is needed to establish that potential,” she says.
When these cell changes occur is important, she explains, because ciliary changes that happen in tissue cells will only affect that particular tissue. In contrast, ciliary changes that happen in neoblasts have the potential to affect many types of tissues.
“It is important to know that MLL1/2 has the ability to set up later events, because that opens up a whole new way of thinking. For example, cilia genes have been implicated in heart defects, but it is not necessarily because cardiac cells have cilia; it’s because the change happened at some earlier stage in development,” Duncan says. “It seems like an important piece of the puzzle to understand that this enzyme can affect the whole group of genes that are involved in cilia. It is not just a single gene; it’s a whole collection of them.”
Conducting the study in vivo provided a “nice, clean connection to the biology associated with these enzymes,” compared to studying them in a petri dish, Duncan adds.
In an eLife paper published online Oct. 12, first author Kimberly Tu, Ph.D., also in the Sánchez Alvarado lab, and colleagues investigate how neoblasts develop into epidermal cells, which make up the worm’s skin. The process involves a series of steps in which different genes are expressed at each stage. The researchers found that a gene called egr-5, which encodes a transcription factor, controls the expression of these marker genes, and is highly expressed when cells begin to differentiate into epidermal cells. When the activity of egr-5 was reduced, it blocked the cells from differentiating properly, and they were unable to make mature skin cells.
“This generates a breach in the integrity of the epidermis,” Tu says. “Eventually the animals will die because they fail to make new epidermal cells.”
The breach also signals a stress response in the planaria, causing the neoblasts to over proliferate and differentiate into other cells including neurons and gut cells. The findings uncover a critical role for egr-5 in the development of epithelial cells, and shed light on the biological complexity at work in this seemingly simple organism.
Additional Stowers authors in Duncan’s study include Chris W. Seidel, Ph.D., Alex D. Chitsazan, M.S., and Alejandro Sánchez Alvarado, Ph.D. Stowers authors involved in Tu’s study include Li-Chun Cheng, Ph.D., Hanh T.K. Vu, Ph.D., Jeffrey J. Lange Ph.D., Sean A. McKinney Ph.D., Chris W. Seidel, Ph.D., and Alejandro Sánchez Alvarado, Ph.D.
The work was funded by the Stowers Institute for Medical Research, the Howard Hughes Medical Institute, and a grant from the National Institute of General Medical Sciences of the National Institutes of Health (NIH R37GM057260). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Lay Summary
Planaria are tiny (about the size of a toenail clipping), aquatic flatworms, most often found in standing water. Though humble in size and appearance, they are one of nature’s wonders. Planaria have the ability to regenerate from a small scrap of tissue, and have an abundance of adult stem cells, called neoblasts, that can specialize, or differentiate, into other cell types. Two new studies from the Stowers Institute shed light on some of the intricate processes at work when planarian neoblasts differentiate into skin cells.
In a study published in the Dec. 17 online issue of Cell Reports, Elizabeth Duncan, Ph.D., identifies how the enzyme MLL1/2 affects the development of planarian cilia, the microscopic, hair-like-structures on the organism’s skin that help it swim. Without the enzyme, planaria lose their cilia and stop swimming. Duncan’s discovery suggests that defects in the process of building cilia may begin earlier than thought, a finding that has potential implications for the detection of a broad range of human health conditions.
Kimberly Tu, Ph.D., and colleagues found that a gene called egr-5 is important and plays a key role in helping neoblasts differentiate into skin cells. When the activity of egr-5 was reduced, it blocked neoblast daughter cells from differentiating properly, and they did not make mature skin cells. The findings uncover the critical role of egr-5 in the development of skin cells, and illustrate the complexity of this seemingly simple organism.
About the Stowers Institute for Medical Research
The Stowers Institute for Medical Research is a non-profit, basic biomedical research organization dedicated to basic research – the critical first step in the quest for new medical diagnostics, therapies and treatments. Jim Stowers, founder of American Century Investments, and his wife, Virginia, opened the Institute in 2000. Since then, the Institute has spent over one billion dollars in pursuit of its mission.
Currently, the Stowers Institute is home to 500 researchers and support personnel, over 20 independent research programs, and more than a dozen technology development and core facilities.
In The News

07 January 2026
From the Journal of Cell Science, Investigator Kamena Kostova named a 'Cell Scientist to Watch'
Read Article
#Stowers25: Celebrating 25 Years
06 January 2026
Alejandro Sánchez Alvarado, Ph.D., reflects on a year of discovery, gratitude, and the community that helps support our mission.
Read Article
In The News
01 January 2026
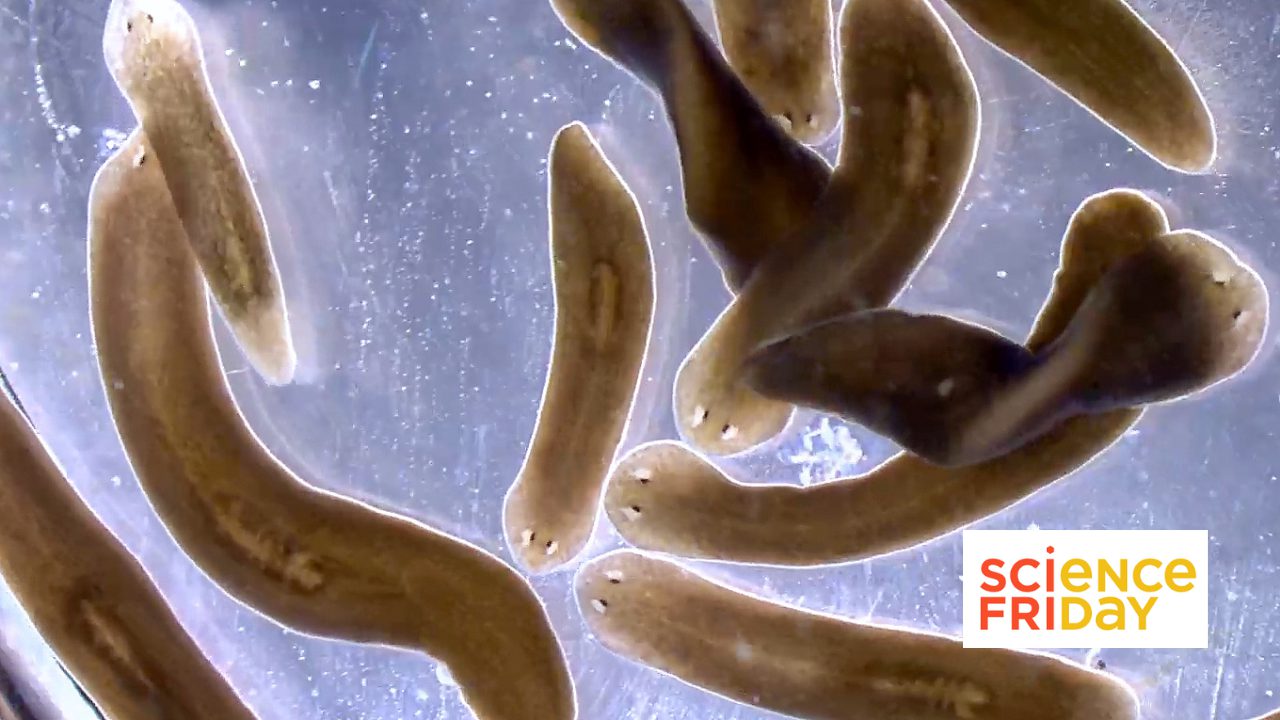
From Science Friday, President and CSO Alejandro Sánchez Alvarado talks about the science of regeneration and the biology lessons we can carry into the new year.
Read Article
